Oral HPV: What You Need to Know
Leggi in Italiano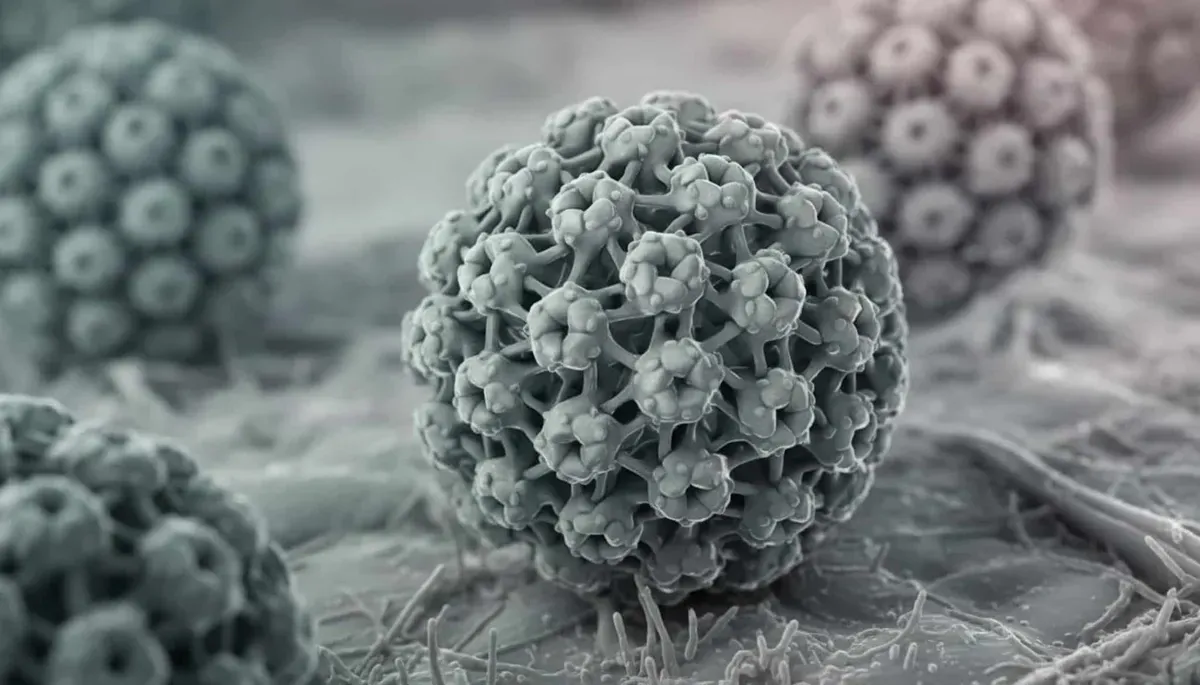
In brief — Oral HPV affects 7% of adults. Most infections resolve, but persistent ones cause oropharyngeal carcinomas that are steadily increasing. Porphyromonas gingivalis facilitates HPV infection by altering the epithelial barrier and suppressing local antiviral immunity. Periodontal biofilm control is also cancer prevention.
Human Papillomavirus (HPV) is not only a matter for gynaecologists. In our daily work we increasingly see lesions in patients’ mouths attributable to this extremely common virus.
What HPV is
HPV is a family of over 150 viruses of the same family (https://www.hpv.org.nz/about-hpv/hpv-strains).
It is the most common sexually transmitted infection.
It is typically contracted through direct skin contact during intimate relations with an infected individual. Viral transmission is possible during vaginal or anal penetration, and through oral sex. It is important to note that condoms do not offer complete protection against HPV, since the virus can infect anatomical regions immediately adjacent to and not covered by the condom.
Most HPV infections resolve on their own within one to two years thanks to the efficient work of the immune system.
Persistent infections with high-risk strains can cause cancer of the mouth and pharynx (throat). The incidence of these tumours has been steadily increasing for decades. Oral cancer has now surpassed even better-known cancers such as melanoma in frequency.
The spread
Recent data show that approximately seven per cent of adults in the United States have an oral HPV infection. It is logical to think that in Europe, where (at least for now) lifestyles are not dissimilar, the statistics are similar.
Fortunately, high-risk strains affect only about one per cent of the population. Men are significantly more likely than women to contract oral HPV. Prevalence peaks occur in two age groups: between thirty and thirty-four, and between sixty and sixty-four.
How oral HPV is transmitted
The main route is oral sex. The virus can also spread through deep kissing with saliva exchange, but this is less common. Vertical transmission from mother to child during birth is rare.
What we do not see
The problem is this: most oral HPV infections are completely asymptomatic. When lesions appear, they can present as small bumps or growths, white or red patches, persistent sore throat, difficulty swallowing, ear pain, enlarged lymph nodes.
The most characteristic lesion is oral papilloma, a benign cauliflower-like pointed growth that typically appears on the soft palate, uvula or tongue. It has a distinctive appearance.
HPV beyond the oral cavity
HPV is not limited to mouth and throat. The virus shows strong affinity for stratified squamous epithelia throughout the body. The uterine cervix remains the most studied site. And it is also the one with the most direct link to the virus: without HPV, the tumour does not develop. Indeed, high-risk strains cause ninety-nine per cent of cervical carcinomas. Screening with Pap smears and HPV tests has drastically reduced mortality in countries with effective screening programmes.
The anogenital region is another frequent and important target. HPV causes vulvar, vaginal, penile and ano-rectal carcinomas (70%). Ano-rectal carcinoma shows increasing incidence, particularly in men who have sex with men and in immunocompromised individuals. Ano-rectal carcinoma incidence rates in these populations approach those of cervical carcinoma in unvaccinated women.
Low-risk strains, primarily HPV-6 and HPV-11, cause genital warts. These benign lesions are highly contagious and can occur on external genitalia, perineum and perianal region. Rarely, children born to mothers with active warts can develop recurrent respiratory papillomatosis, a condition in which papillomas grow in the larynx and airways.
The skin can harbour cutaneous HPV. These different strains cause common warts on hands and feet. Some cutaneous strains are associated with non-melanoma skin cancer, especially in immunocompromised patients. The evidence here is less robust than for anogenital and oropharyngeal tumours.
The immune system determines the course of infection. Most immunocompetent individuals clear the virus. Those with a compromised immune system, due to HIV, organ transplantation or immunosuppressive therapies, show higher rates of persistent infection and progression to cancer. This applies to all anatomical sites.
Porphyromonas gingivalis and HPV: a dangerous alliance
Periodontal disease is not just a matter of bone loss and pockets. Porphyromonas gingivalis, the keystone pathogen in chronic periodontitis, can influence the persistence and progression of oral HPV. The evidence comes from epidemiological and laboratory studies.
Patients with periodontitis show higher rates of oral HPV infection compared to those with healthy gums. Cohort studies have found a significant correlation between the presence of Porphyromonas gingivalis and high-risk HPV in the oral cavity. The relationship is not coincidental.
Porphyromonas gingivalis produces gingipains, enzymes that degrade host proteins. These proteases alter the epithelial barrier and facilitate the entry and persistence of HPV in epithelial cells. The bacterium essentially creates a permissive environment for the virus.
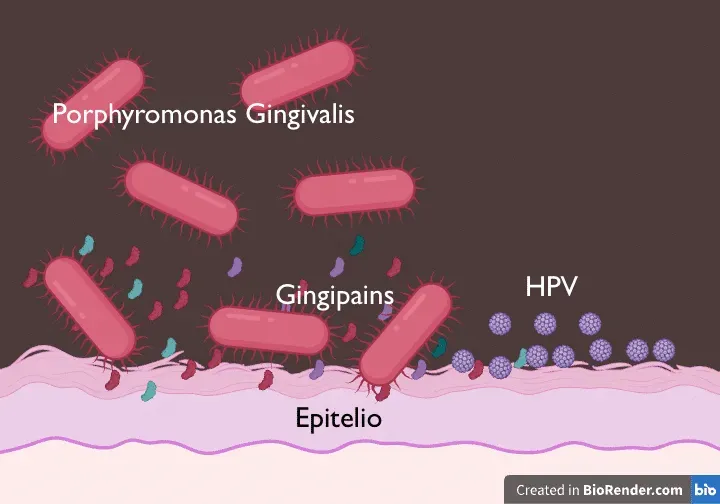
The chronic inflammation caused by periodontitis (or periodontal disease) plays a central role. Porphyromonas gingivalis stimulates the production of pro-inflammatory cytokines: interleukin-6, interleukin-8, tumour necrosis factor alpha. This chronic inflammatory state, among other things, suppresses local antiviral immunity. The immune system, engaged in fighting the bacterial infection, is less effective at eliminating HPV.
In vitro research demonstrates even more direct mechanisms. Porphyromonas gingivalis can increase the production of HPV oncoproteins E6 and E7. These viral proteins inactivate the tumour suppressors p53 and pRb. The result is uncontrolled cell proliferation, with suppression of the natural apoptosis (cell death) of tumour cells. The bacterium, therefore, not only facilitates infection but may accelerate malignant transformation.
Studies on HPV-positive oropharyngeal carcinomas (mouth and throat) frequently show the presence of Porphyromonas gingivalis in tumour tissues. Co-presence does not prove causality but suggests synergy. The bacterium may contribute to progression from infection to dysplasia and finally to invasive carcinoma.
For us dentists who work in the mouth every day, this means something concrete. Periodontal health is not separate from oral cancer risk. Treating periodontitis is not just about preserving bone and teeth. It is cancer prevention.
Bacterial biofilm control reduces chronic inflammation. It reduces Porphyromonas gingivalis levels. It potentially reduces the risk of HPV persistence and progression to cancer. Direct evidence of this protective effect in humans is still lacking. But the data strongly suggest this direction.
The link with cancer
HPV-related oropharyngeal carcinomas have distinct characteristics. They tend to appear at the base of the tongue and in the tonsils. Fortunately, they respond better to treatment than HPV-negative tumours. They are on the rise, particularly among non-smoking males. HPV-positive oropharyngeal carcinoma now accounts for approximately seventy per cent of all oropharyngeal carcinomas.
Prevention
The HPV vaccine protects against the nine HPV types most commonly associated with cancers and genital warts. It was originally recommended for pre-adolescents aged eleven to twelve. It is now approved for adults up to forty-five. It is most effective when administered before exposure to the virus. Studies suggest it can reduce rates of oral HPV infection.
Classically, data indicate the vaccine is ineffective on existing lesions. However, this finding is challenged by reports of HPV lesion regression after vaccination. (See also this article on vaccines)
Recent articles demonstrate virus clearance from the host following vaccine administration. Furthermore, vaccination has a protective effect against recurrence of cervical tumours.
What we tell patients
When patients ask about oral HPV, a practical approach is needed. We acknowledge their concern. Yes, HPV can affect mouth and throat. We provide context. Most infections resolve on their own and never cause problems.
We discuss risk factors: the number of oral sex partners, smoking as a cofactor, a weakened immune system, untreated periodontal disease. We emphasise prevention: HPV vaccination for an ever-broader population, treatment of any periodontitis (which affects 60% of the population). Regular mouth and throat examinations with inspection of all mucosal surfaces. Screening tests, which now make prevention more immediate.
Any persistent lesion or pharyngeal symptom requires immediate referral to an otolaryngologist.
References
- Zaidi SE, Hans S, Colombier MA, Contrera KJ, Farfour E, Rigal T, Baudouin R. Impact of the Microbiome on Onset and Prognosis of Oropharyngeal Squamous Cell Carcinoma. Head Neck. 2025;47(10):2911-2920. https://doi.org/10.1002/hed.70002
- Lim YX, D’Silva NJ. HPV-associated oropharyngeal cancer: in search of surrogate biomarkers for early lesions. Oncogene. 2024;43(8):543-554. https://doi.org/10.1038/s41388-023-02927-9
- Sánchez-Ponce Y, Fuentes-Pananá EM. The Role of Coinfections in the EBV-Host Broken Equilibrium. Viruses. 2021;13(7):1399. https://doi.org/10.3390/v13071399
- Shen J, Lin H, Mo K, Liang Z, Zhang Y, Quan H, Wang X, Zhang C, Chen C. Bidirectional roles of neutrophil extracellular traps in oral microbiota carcinogenesis: A systematic review. Transl Oncol. 2025;56:102361. https://doi.org/10.1016/j.tranon.2025.102361
- Farhad SZ, Karbalaeihasanesfahani A, Dadgar E, Nasiri K, Esfahaniani M, Nabi Afjadi M. The role of periodontitis in cancer development, with a focus on oral cancers. Mol Biol Rep. 2024;51(1):814. https://doi.org/10.1007/s11033-024-09737-6
- Constantin M, Chifiriuc MC, Mihaescu G, Vrancianu CO, Dobre EG, Cristian RE, Bleotu C, Bertesteanu SV, Grigore R, Serban B, Cirstoiu C. Implications of oral dysbiosis and HPV infection in head and neck cancer: from molecular and cellular mechanisms to early diagnosis and therapy. Front Oncol. 2023;13:1273516. https://doi.org/10.3389/fonc.2023.1273516
- Saikia PJ, Pathak L, Mitra S, Das B. The emerging role of oral microbiota in oral cancer initiation, progression and stemness. Front Immunol. 2023;14:1198269. https://doi.org/10.3389/fimmu.2023.1198269
- Li R, Xiao L, Gong T, Liu J, Li Y, Zhou X, Li Y, Zheng X. Role of oral microbiome in oral oncogenesis, tumor progression, and metastasis. Mol Oral Microbiol. 2022;38(1):9-22. https://doi.org/10.1111/omi.12403
- Castañeda-Avila MA, Pérez CM, Vivaldi J, Díaz-Toro EC, Ramos-Cartagena JM, Andriankaja OM, Ortiz AP. Oral Inflammation and Human Papilloma Virus Association among Hispanics. Int J Dent. 2023;2023:7247976. https://doi.org/10.1155/2023/7247976
- Ortiz AP, González D, Vivaldi-Oliver J, Castañeda M, Rivera V, Díaz E, Centeno H, Muñoz C, Palefsky J, Joshipura K, Pérez CM. Periodontitis and oral human papillomavirus infection among Hispanic adults. Papillomavirus Res. 2018;5:128-133. https://doi.org/10.1016/j.pvr.2018.03.003
- Zheng Q, He M, Mao Z, Huang Y, Li X, Long L, Guo M, Zou D. Advancing the Fight Against Cervical Cancer: The Promise of Therapeutic HPV Vaccines. Vaccines. 2025; 13(1):92. https://doi.org/10.3390/vaccines13010092
- Wang, R., Huang, H., Yu, C., Li, X., Wang, Y., & Xie, L. (2024). Current status and future directions for the development of human papillomavirus vaccines. Frontiers in immunology, 15, 1362770. https://doi.org/10.3389/fimmu.2024.1362770
FAQ
What exactly is HPV and why is it important beyond gynaecology? HPV, or Human Papillomavirus, is a family of over 150 viruses representing the most common sexually transmitted infection. It is also relevant to diagnosis and prevention in general medicine due to its widespread nature and associated complications.
How is oral HPV transmitted and what are the main risk factors? Oral HPV is primarily transmitted through oral sex, while deep kissing with saliva exchange is less common; risk factors include the number of sexual partners, smoking, a weakened immune system and the presence of untreated periodontal disease.
What are the most common symptoms and visible lesions of oral HPV? Most oral HPV infections are asymptomatic, but when they manifest, they can present as small bumps, growths, white or red patches, persistent sore throat, ear pain, enlarged lymph nodes, or oral papilloma — a cauliflower-like growth.
How can HPV be linked to oral cancers and what are the potential benefits of prevention? HPV, particularly certain high-risk strains, can cause cancers of the mouth and pharynx, with oropharyngeal carcinomas being most common; prevention through vaccination and regular check-ups can counter this spread and drastically reduce the risk of developing cancer.
What prevention strategies should be communicated to patients regarding HPV? HPV vaccination is recommended, which protects against the types most commonly associated with cancers and genital warts, along with regular mouth and throat check-ups; it is essential to inform patients about risk factors and prevention methods, including condom use and good oral care.
FAQ
- What exactly is HPV and why is it important beyond gynaecology?
- HPV, or Human Papillomavirus, is a family of over 150 viruses representing the most common sexually transmitted infection. It is also relevant to diagnosis and prevention in general medicine due to its widespread nature and associated complications.
- How is oral HPV transmitted and what are the main risk factors?
- Oral HPV is primarily transmitted through oral sex, while deep kissing with saliva exchange is less common; risk factors include the number of sexual partners, smoking, a weakened immune system and the presence of untreated periodontal disease.
- What are the most common symptoms and visible lesions of oral HPV?
- Most oral HPV infections are asymptomatic, but when they manifest, they can present as small bumps, growths, white or red patches, persistent sore throat, ear pain, enlarged lymph nodes, or oral papilloma — a cauliflower-like growth.
- How can HPV be linked to oral cancers and what are the potential benefits of prevention?
- HPV, particularly certain high-risk strains, can cause cancers of the mouth and pharynx, with oropharyngeal carcinomas being most common; prevention through vaccination and regular check-ups can counter this spread and drastically reduce the risk of developing cancer.
- What prevention strategies should be communicated to patients regarding HPV?
- HPV vaccination is recommended, which protects against the types most commonly associated with cancers and genital warts, along with regular mouth and throat check-ups; it is essential to inform patients about risk factors and prevention methods, including condom use and good oral care.
Looking for a specialist?
Parodontologia a Frosinone →Diagnosi e trattamento della parodontite nello Studio Denti Più
Need a professional opinion?
Book an appointment at Dr. Bruschi's practice in Frosinone. First visit includes full diagnosis and personalised treatment plan.
Stay Updated
New articles on periodontology, implantology and oral surgery — delivered to your inbox.
Comments
Loading comments...
Leave a comment